What are tonsils & adenoids?
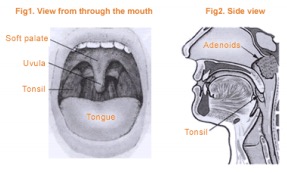
Tonsils are lumps of tissue on both sides of the throat and the adenoids are similar tissue behind the palate. Tonsils and adenoids serve to develop immunity until
the age of 2. Tonsils and adenoids also trap bacteria and viruses entering through the throat and nose, producing antibodies to help fight infections. Long term studies show that removing tonsils and adenoids have no long term consequences to a person’s ability to fight infections in the future.
What is tonsillitis?
Tonsillitis refers to inflammation of the pharyngeal tonsils. The inflammation may involve other areas of theback of the throat including the adenoids and the lingual tonsils (areas of tonsil tissue at the back of the tongue). There are several variations of tonsillitis: acute, recurrent, and chronic tonsillitis and peritonsillar abscess (quinsy).
What are the symptoms of tonsillitis?
The type of tonsillitis determines what symptoms will occur:
* Acute tonsillitis: Patients have a fever, sore throat, foul breath, dysphagia (difficulty swallowing), odynophagia (painful swallowing), and tender cervical lymph nodes.
* Recurrent tonsillitis: This diagnosis is made when an individual has multiple episodes of acute tonsillitis in a year.
* Chronic tonsillitis: Individuals often have chronic sore throat, bad breath, tonsillitis, and persistently tender cervical nodes.
* Peritonsillar abscess: Individuals often have severe throat pain, fever, drooling, foul breath, trismus (difficulty opening the mouth), and muffled voice quality, such as the “hot potato” voice.
Treatment for tonsillitis
Tonsillitis is usually treated with a regimen of antibiotics. Fluid replacement and pain control are important. Hospitalisation may be required in severe cases, particularly when there is airway obstruction. When the condition is chronic or recurrent, a surgical procedure to remove the tonsils, tonsillectomy, is often recommended.
What is Sleep Disordered Breathing (SDB)?
The commonest symptom of sleep disordered breathing is snoring. Approximately 10 percent of children are reported to snore. Ten percent of these children (one percent of the total paediatric population) have obstructive sleep apnoea. When an individual, young or old, obstructs breathing during sleep, the body perceives this as a choking phenomenon. The heart rate slows, the sympathetic nervous system is stimulated, blood pressure rises, the brain is aroused, and sleep is disrupted. In most cases a child’s vascular system can tolerate the changes in blood pressure and heart rate. However, a child’s brain does not tolerate the repeated interruptions to sleep, leading to a child that is sleep deprived, cranky, and ill behaved.
Consequences of untreated paediatric sleep disordered breathing:
* Snoring: A problem if a child shares a room with a sibling and during sleepovers.
* Sleep deprivation: The child may become moody, inattentive, and disruptive both at home and at school. The child will lack energy.
* Abnormal urine production: SDB also causes increased nighttime urine production, and in children, this may lead to bedwetting.
* Growth: Growth hormone (GH) is secreted at night. Low GH secretion may lead to slow growth or development.
* Attention deficit disorder (ADD) Research suggests SBD can be associated with ADD.
A child with suspected SDB should be evaluated by an Ear, Nose & Throat surgeon. If the symptoms are significant and the tonsils are enlarged, the child is strongly recommended for adenotonsillectomy (removal of the tonsils and adenoids or T & A). Conversely, if the symptoms are mild, academic performance remains excellent, the tonsils are small, and puberty is imminent (tonsils and adenoids shrink at puberty), it may be recommended that SDB be treated only if matters worsen.
Treatment for sleep disordered breathing
Adenotonsillectomy achieves a 95% percent success rate for childhood SDB. A failure rate is due to either adenoid re-growth or immature brain triggering mechanisms for breathing.